Do you remember your IUD insertion? Pain can range from “ouch, that was annoying” to “DEATH TAKE ME NOW.” Even if the discomfort was “code red” status, there’s a silver lining. The procedure is super quick, and once it’s in, your uterus is a baby-free zone for the next 3 to 10 years (depending on the IUD).
But there’s a small downside. Sometimes, an IUD string goes MIA. This can be stressful, especially if you’re sexually active and afraid of pregnancy. Here’s what you need to know about your IUD string and why you may not feel it.
When an IUD is inserted, two plastic strings — part of the IUD — are left sticking out of your cervix. The string may feel foreign at first, but it’s totally harmless.
In fact, it can offer you a sense of relief. When you feel the string, you know your womb is on lockdown. So when that string vanishes, your instinct might be to panic. If that’s the case, you’re not alone. A recent study showed as many as 18 percent of women cannot feel their IUD strings.
Here are some potential causes.
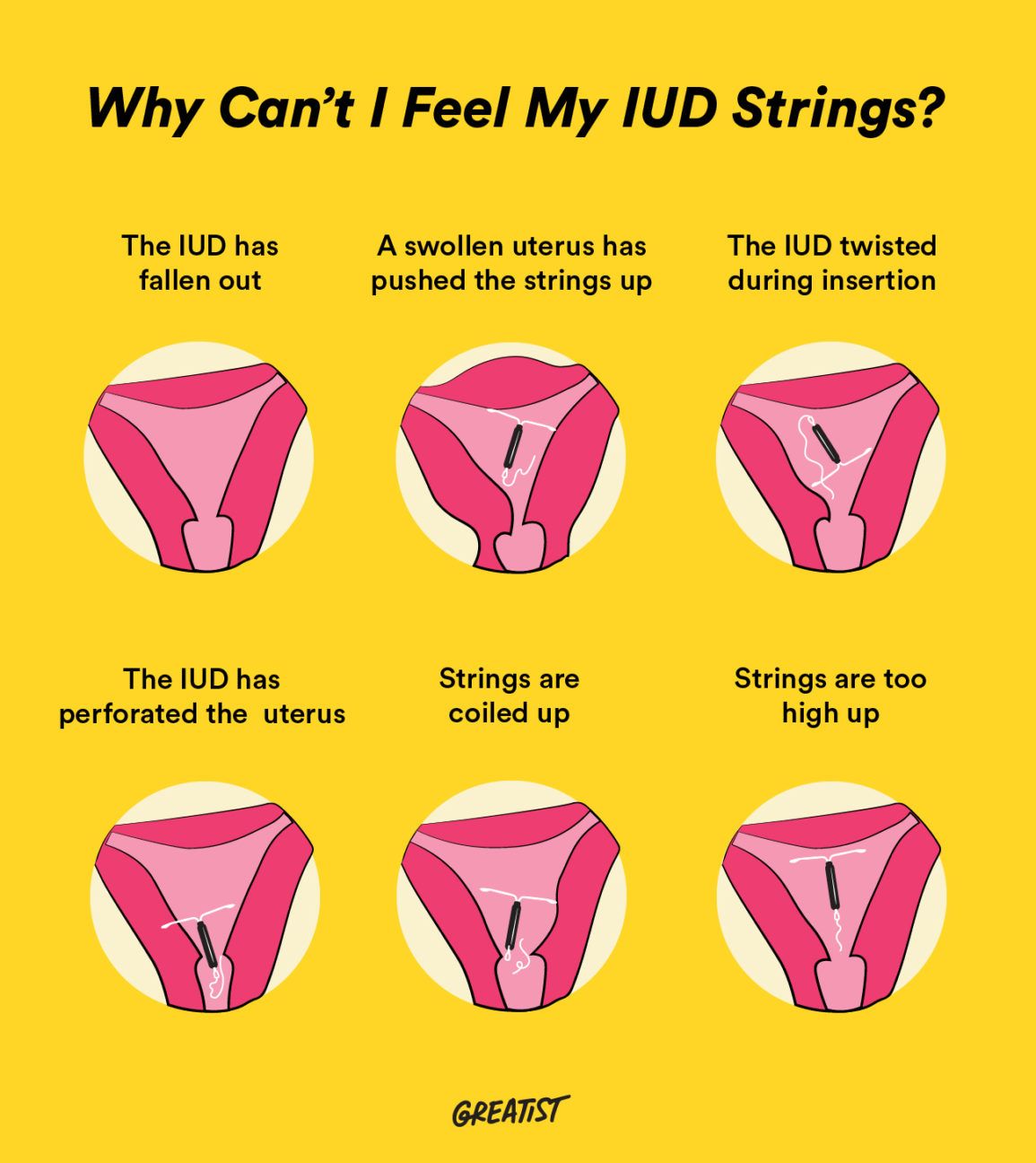
Short strings attached
There’s a chance your IUD string is still there, but it’s too high up your vag to be felt. Maybe your fingers aren’t long enough to reach it, or your doctor cut the string too short.
In this scenario, your IUD is still totally functional. To play it safe, make a doctor’s appointment to make sure it’s in the right position.
It curled up
Occasionally, IUD strings like to play hide-and-seek in your vaginal tissue. The string coils into your endocervical canal — an area in your cervix — so you can’t feel it.
Thankfully, your next period may push the strings back to their original position. If not, check in with your doctor.
When IUDs go rogue
IUD expulsion only occurs in 3 to 10 percent of all patients and depends on several factors, so it’s fairly rare. If it does happen, it’s usually within the first year after insertion. Here are some risk factors to look out for:
- previous IUD expulsion
- you’re under the age of 20
- you recently delivered a baby
- you have a very heavy menstrual flow
- you experience ultra intense period cramps
- you’ve never given birth
- you had it inserted immediately after a second-trimester abortion
It stabbed me!
Perforation happens when your IUD pokes through your uterus or cervix. Perforation is rare; according to the American College of Obstetricians and Gynecologists, it only happens in 0.11 percent (1.1 per 1,000) of copper IUD insertions, and in 0.14 percent (1.4 per 1,000) of hormonal IUD insertions.
You’re more at risk of perforation if you’ve recently delivered or if you’re breastfeeding.
Your uterus got swole
The uterus was designed to grow a baby, so expansion is its jam. But sometimes the uterus may enlarge for other reasons. A common perpetrator behind uterine enlargement are uterine fibroids.
An estimated 80 percent of women will develop a uterine fibroid at some point in her life. Most of the time they’re benign and basically harmless, but sometimes they can make your uterus swell, repositioning your IUD.
Your IUD flip-flopped
There’s a chance your IUD rotated during insertion. Malposition can occur for a few reasons. If your uterine cavity is too small, the IUD may not fit properly. Your body may try to evict the device, especially while you’re on your period.
Or an inexperienced medical professional may have inserted it incorrectly, causing it to tilt inside the uterus. That’s why it’s important to ask for a sonogram to confirm the IUD is in the correct position after the procedure.
When it comes to IUDs, you have to listen to your body. If you have a hormonal IUD (like Liletta, Kyleena, Skyla, or Mirena), your periods may become shorter and lighter after insertion.
If you notice a huge change in your blood flow — especially if you have extremely heavy bleeding — schedule a checkup. There’s a chance your IUD has fallen out or is in a weird position.
Certain symptoms can point to a larger issue like infection or perforation.
Go to the doctor ASAP if you’re experiencing:
- abnormal fluid, blood, or smells coming from your vagina
- severe cramping
- chills and fever
Your doctor will provide a pelvic exam to see if they can feel your IUD strings.
They may use a cytobrush to help them find the strings. Or, they’ll use a magnifying device called a colposcope to give them a better look. It all sounds scary, but fear not. It feels like a pap smear.
They may do an internal ultrasound if they can’t find the strings. You probably had this done when your IUD was first inserted to make sure it was placed properly. If your IUD doesn’t appear, there’s a solid chance it’s gone AWOL.
If your IUD is missing, your doctor may do an X-ray to see if it snuck out of your uterus and entered your abdominal cavity.
In the rare instance that your uterus has been perforated, you will have to have the IUD surgically removed. It’s most likely just in the wrong position though, and can be easily repositioned or replaced by your doctor.
In the interim, you may want to use an another for of birth control. And, if there are changes in your bleeding or concern for pregnancy, a pregnancy test may be in order.
You should check your IUD string every month to make sure everything is still hunky-dory.
To DIY string check:
- Wash your hands.
- Sit or lie down in a comfortable position.
- Insert your index and/or middle finger into your vagina. You should feel your cervix about 1 to 2 inches up.
- Feel for the string (but be careful not to tug on it when withdrawing your fingers).
If you can’t feel your IUD string, use other forms of contraception until you can get to the doctor.
No matter what the reason is for using an IUD, you should be proud of yourself. You’re taking your health and wellbeing seriously.
If you can’t feel your IUD strings, don’t panic — the IUD most likely shifted positions and can easily be adjusted. Follow the steps from this article and make an appointment with your gyno. It’s always better to play it safe than to be left unprotected.

