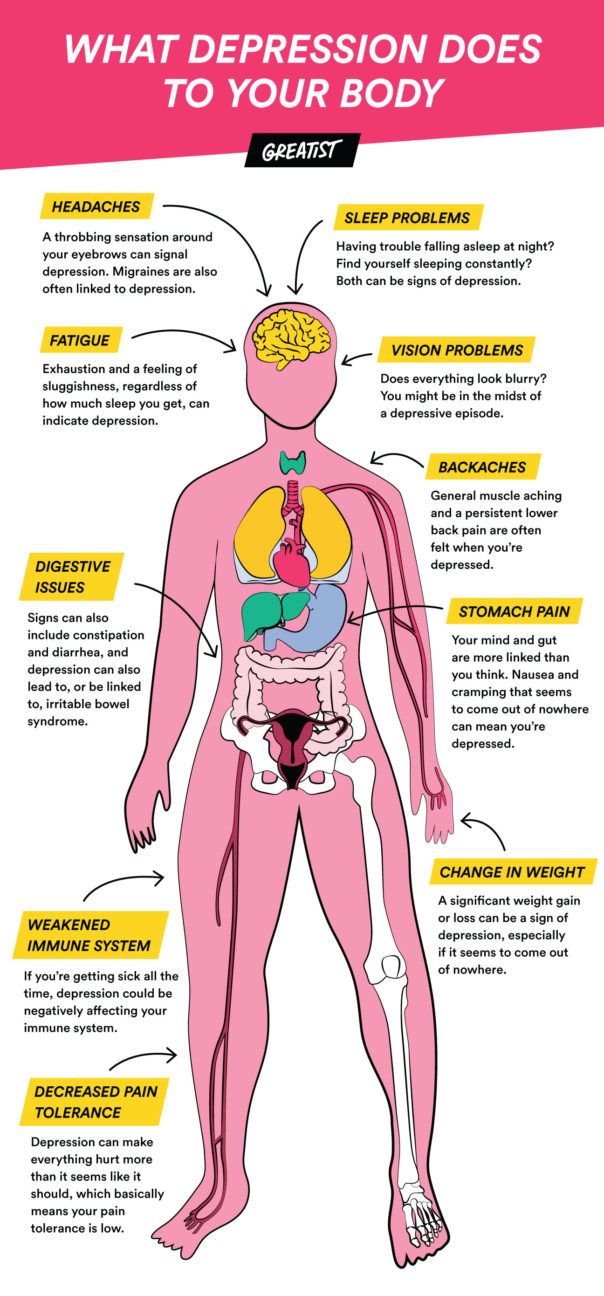
Have you ever noticed how the words we use to describe depression often carry a physical quality? Phrases like feeling fatigued, weighed down, or like your heart aches are often our go-tos.
And while the emotional element of depression is very real, these words are more accurate than some may realize. After all, depression comes with plenty of physical side effects too.
Whether you have a diagnosis or suspect you might be living with depression, understanding the physical component of this disorder can seriously improve your quality of life.
Here’s exactly how depression affects your body — and what you can do about it.
There’s plenty of research that backs up the fact that depression affects more than just your mind. Physical symptoms can indicate that you’re about to enter a depressive period, or they can be signs of more serious types of depression.
That said, don’t assume that these symptoms alone (which can also be attributed to many other things) mean you’re depressed. If they go along with lingering feelings of unhappiness, hopelessness, and suicidal thoughts, that could mean they’re part of depression.
And don’t forget…
If you’re experiencing suicidal thoughts, help is always available. The National Suicide Prevention Lifeline is available 24 hours a day, so don’t hesitate to call: 1-800-273-8255. You can also always call or visit your nearest emergency room to speak with a mental health professional on hand.
If you prefer to text, reach the Crisis Text Line by texting “HOME” to 741-741.
1. Headaches
Tension headaches are often associated with depression. You can expect a mild to moderate throbbing sensation around your eyebrows or the middle of your head, or even in your neck.
Migraines are also associated with depression, but there’s a difference: It can be unclear whether depression is causing the migraine, or the migraine is causing depression.
A migraine attack will happen suddenly, out of nowhere, and can last for a few hours or even days. Migraines can leave you extremely sensitive to light and sound, nauseous, and unable to complete basic tasks. They often happen before depression occurs.
2. Fatigue
Many depressed people report feeling some type of fatigue, whether it’s utter exhaustion no matter how much sleep they’re getting, or a sluggish feeling that leaves them incapable of doing much.
This kind of fatigue isn’t just your average, “I didn’t get enough sleep last night” exhaustion. It’s more like, “I can’t concentrate, focus, or enjoy anything” exhaustion.
3. Stomach pain
There are so many reasons you could experience stomach pain that it’s easy to write it off as something completely unrelated to depression. But research has found there’s a definite brain and gut connection, meaning depression (and anxiety) could be to blame for any stomach issues.
According to Harvard Medical School, the brain has a direct effect on the stomach and can easily cause pain — just like stomach pain can, in turn, cause depression.
4. Digestive distress
It’s not just your stomach that can feel out of sorts when you’re depressed — the same brain-gut connection that can cause nausea can also cause digestive issues like irritable bowel syndrome (IBS) or other similarly fun types of intestinal distress.
Digestive problems can also cause depression — research has shown that microbiota in your gut can affect your mood in a serious way. Look out for constipation or diarrhea that go along with emotional depression symptoms as well.
5. Back aches
Back pain or a general achy feeling that seems to arrive for no particular reason isn’t just the product of an aging body (hey, we all get older!). Back pain is a common physical symptom of depression.
One study actually found a direct link between back aches and depression — discovering that persistent back pain increases the risk of depression, and people who live with depression are 60 percent more likely to develop back pain.
Some research suggests that inflammation in the body can affect our minds and emotions, which could potentially explain this link.
6. Vision issues
It’s hard to ignore worsening eyesight and a tendency for everything around you to look blurry. Sure, you might need glasses, but this could also be your body’s way of telling you that you’re depressed.
Research shows that persistent stress may lead to a loss in vision, and one study even found that vision loss and depression are significantly linked for older adults.
7. Weakened immune system
Constantly sick? Can’t seem to get rid of that cold you’ve had for the past several weeks? Consider your emotional symptoms.
Research has found that depression can actually weaken your immune system, leaving you more susceptible to illness.
Why? Excess stress that comes with depression may lead to an inflammatory response that could change the way your brain works and responds to foreign invaders (aka germs, bacteria, and viruses).
8. Change in weight or appetite
Gaining or losing weight can indicate depression, and no, we’re not talking about the five pounds that seems to come and go whenever it pleases.
This would be a significant change in your weight that is noticeable to those around you, and doesn’t seem to be a result of a new diet and exercise program.
Some people who experience depression don’t find food appetizing, and end up losing a lot of weight from not eating.
Others may end up eating more than normal (this is is known as emotional eating) causing them to gain weight (one study has even linked obesity to depression).
It is also common for people with eating disorders, such as anorexia nervosa, to also have depression.
If you’re noticing weight fluctuations or struggling with an eating disorder, set up a quick chat with your healthcare provider. They can give you the tools to get back to eating healthfully and feeling better.
9. Sleep problems
Some people with depression want to sleep all the time, even if it doesn’t leave them feeling rested. Others may find it difficult to sleep at all, no matter the time of night or day.
One thing is for sure: research has found a very strong link between sleep issues and depression, with one study saying that about three quarters of depressed patients also experience sleep issues.
10. Decreased pain tolerance
Depression can leave you feeling like every little thing hurts more than it should — and, unfortunately, that’s normal. Studies have found that there’s a link between depression and a decreased pain tolerance, so no, it’s probably not all in your head.
Depression is not one-size-fits-all. There are different kinds of depression that also come with their own set of symptoms.
Anxiety disorder
Anxiety disorders, including panic disorders, generalized anxiety disorder, phobias, or social anxiety, can have symptoms that are really similar to depression. But other symptoms that depression may not share include:
- rapid breathing or shortness of breath
- increased heart rate
- sweating
- trembling or shaking
Clinical/severe depression
Severe depression, known as major depressive disorder (MDD), shares all of the same physical symptoms as depression, although they may all be felt on a larger scale, or you may feel more of them. On top of that, you may also experience:
- low sex drive
- changes to your menstrual cycle
Postpartum depression
Any woman who has recently given birth is at risk for postpartum depression, or MDD with peripartum onset.
The physical symptoms are very similar to serious depression — it’s the emotional symptoms that can differ, as they often relate to feelings regarding motherhood and the new baby.
Premenstrual dysphoric disorder
When PMS goes from an annoyance to something that is significantly affecting your mood and life, you may have premenstrual dysphoric disorder (PMDD).
This comes with the depression symptoms we’ve discussed, and can also include:
- muscle spasms
- hot flashes
- dizziness
- fainting
- respiratory complaints
- painful menses
- decreased libido
- easy bruising
- fluid retention and swelling
- heart palpitations
- acne
- pelvic pressure
- skin disorders like cold sores
Seasonal affective disorder
If depression starts to hit as winter begins, and goes away as the ice is beginning to thaw, you may have seasonal affective disorder (commonly known as SAD, and also called MDD with seasonal pattern).
SAD will result in:
- lower energy (maybe more so than just regular depression)
- hypersomnia
- intense food cravings
- a decreased sex drive
No one wants to be depressed, and getting the right kind of treatment can be tough. It can be hard for a person with depression to even talk themselves into getting help.
Treatment methods can require a bit of trial and error, but it’s worth it.
Speak with your healthcare provider to create a personalized treatment plan that works for your specific symptoms. There are tons of treatment options available (and no, they don’t all involve medication!).
Talk therapy
Seeing a therapist, counselor, or psychologist can help lessen feelings of depression, in turn decreasing the physical symptoms as well.
According to Harvard Medical School, some studies have found that talk therapy is a better way to decrease stomach or gut issues associated with depression than medication alone.
Medications
Antidepressants were made specifically to combat symptoms of depression and anxiety.
Sometimes medication is really the best route there is, especially if you’ve tried talk therapy and have found that it’s not helping like you wish it would.
Medications can make you feel emotionally better and can relieve certain physical symptoms as well.
The only downside to medication is that, while they may relieve some physical symptoms, some may actually cause physical side effects. You may need to try out a few in order to find the best option for you.
Light therapy
Exposure to white light isn’t just helpful for seasonal affective disorder (although this is a huge treatment for anyone affected by SAD). It can also help with any sleep issues associated with depression.
Alternative therapy
You may want to try something like acupuncture or meditation if you’re looking for a different approach to treatment.
Aside from possibly helping with depression, acupuncture can also ease the pain of symptoms that go along with it, like headaches, cramps, muscle aches, and lower back pain.
Natural methods
If medicine and therapy isn’t up your alley, you can try the more natural approach to treatment. This can include: essential oil therapy, exercise, taking supplements, and taking vitamins.
Certain supplements and vitamins may have a positive effect on your mind and body. Exercise can increase your body’s production of endorphins, which can naturally lift your mood.